 On one fairly routine day for a postnatal doula I found myself ringing the doorbell of a potential client. Her baby was 2 months old and she wanted some support with the baby while she rested. As I greeted her and cast my eyes around the house, I could see with a glance that all was not right.
On one fairly routine day for a postnatal doula I found myself ringing the doorbell of a potential client. Her baby was 2 months old and she wanted some support with the baby while she rested. As I greeted her and cast my eyes around the house, I could see with a glance that all was not right.
Usually by 8 weeks in, mothers are getting into the swing of things, feeding is more or less established, baby’s sleep and waking patterns becoming slightly more predictable. Generally by now, they are waving goodbye to their postnatal doulas, not calling one in.
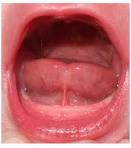
It only took me a moment to get an idea of what had been occurring here. One look at the baby and my heart sunk. There was the characteristic heart-shaped tongue. As I looked more closely I saw the flash of frenulum I have become so familiar with. It was attached right at the tip, tethering his tongue cruelly to the floor of his mouth.
– See more at: https://thebirthhub.co.uk/tongue-tie-stories
That mum never did breastfeed. She had so desperately wanted to and who’s to say if it would have been different if the tie had been released. The issue for me is that no-one gave her the choice.
As doulas it can be hard for us to work out who to listen to when it comes to this controversial subject.
Some say that tongue tie never effects breastfeeding or that it doesn’t even exist. Others that only those that are affecting breastfeeding should be offered division (the use of sterile, round-ended scissors or laser to cut the frenulum so that it no longer tethers the tongue to the floor of the mouth). There is much disagreement on how much frenulum is too much, what breastfeeding problems are due to tongue tie and whether mothers should soldier on for some time to ‘prove’ that breastfeeding support can’t help them, and then and only then, division be offered.
There are many who only look in a baby’s mouth and declare ‘no tongue tie’ but others who say that only by feeling for it do they get a real sense of how the tongue is functioning and that the oral anatomy should always be looked at as just part of a full picture of this dyad and their breastfeeding relationship.
There is argument over the ‘correct’ way to divide the tie and you wouldn’t believe the frothing at the mouth (and I’m not talking about babies here!) that occurs when people start talking about how best to care for the wound after division! There are distinct camps, with people who are pretty darn evangelical about their stance.
Then, of course there are those who say that tongue tie is being over-diagnosed – and why would nature play such a cruel trick. Surely more mothers could breastfeed if they just did it right?
The fact is, the jury is still out.
There is some good evidence for dividing tongue ties. In 2007, an RCT in Southampton found:
“two groups of babies were immediately returned to their mothers for breast-feeding, either after division of the tongue tie or without treatment. During interviews, 21 (78%) of 27 women whose infants received treatment said breast-feeding had improved compared with 14 (47%) of 30 mothers whose infants were not treated. The experiences of 3 women were excluded because of a loss of blinding. The results were statistically significant ( P < .03). Follow-up surveys a day later found that 90% of mothers reported improved feeding, with 3.3% reporting a full resolution of problems. Repeat interviews after 3 months revealed that 90% of the mothers still experienced improved feeding compared with their pre-surgical experiences, but now 55% said that their breast-feeding problems were fully resolved.
The NICE guidelines are pretty positive about mothers being offer this intervention too. But the studies are small and when it comes to WHEN division should be offered, to whom and the techniques that should be used and what, if anything, we should do to the wound afterwards…well, we just don’t know. And the narrative is always couched in terms of what the ‘experts’ should be doing or not doing.
As usual, there just isn’t enough listening to the women going on.
It seems to me that too many people are only looking at the baby and not at how this unique jigsaw puzzle fits together. I am convinced (because I’ve seen it) that you can take a baby with a severely restricted tongue who has caused his mother terrible nipple trauma and give him to another woman to nurse and he will not cause her much, if any, discomfort at all.
Here’s a revolutionary idea – how about we get up front with parents about what we know and crucially, what we don’t know about tongue tie and the effectiveness of dividing it and let them choose?
So, for what it’s worth, here are some of my observations from supporting hundreds of families through tongue tie:
1. Do your research and talk to people. Use your gut and work out what feels sensible to you and what sounds questionable and follow your instincts. If you feel that the tongue tie is causing your problems, keep pushing til you get the support you feel you need. How do you feel about the wound care that some practitioners are advising? Want to know more? Try this article: http://www.analyticalarmadillo.co.uk/2012/12/what-is-appropriate-aftercare-following.html
2. Understand that it is not what the tongue looks like but TONGUE FUNCTION that makes the difference. The tongue needs to do all sorts of clever things to feed effectively, so just being able to extend the tongue beyond the lower gum line is no proof there’s no restriction. There are a million and one other myths about tongue tie, including ‘he can drink from a bottle, so he can’t be tongue tied’ or ‘she’s not in pain so it can’t be tongue tie’. Check out everything everyone ever says to you and take nothing as read.
3. It may be that every tongue tie doesn’t need dividing. Maybe, if you battled on for a few more weeks, this pain or problem might finally disappear. Maybe babies’ mouths grow, MAYBE frenulums stretch and tongue function improves, MAYBE mother and baby work out a way to feed that is effective and comfortable enough to continue. But MOTHERS are the only ones who get to decide what is appropriate. Can she handle this pain/problem for an unspecified amount of time or will she, if nothing is done NOW, pack it in and reach for the bottles? No-one gets to judge her for how she’s feeling now and what she may decide she needs. Dividing a tongue tie can be a timely intervention that can play a part in saving a breastfeeding relationship. Given what a low risk procedure it has been proven to be, why shouldn’t it be freely available?
4. Tongue tie division is a pretty darn safe procedure. In 10,000 divisions in Southampton there has been one mild case of infection.
5. Look at the pros and cons of the different treatment options in your area. NHS? Are there waiting lists? Do they turn away posterior ties? What do they even define as a posterior tie? One that is not attached to the tip of the tongue, or one that is waaaaay back under the mucosal layer on the floor of the mouth? How do they divide the tie? How long are you separated from your baby? What ages of baby will they divide, before advising a general anaesthetic? Do they provide breastfeeding support after the division? And what (if anything) will you be advised to do to the wound afterwards – and how do you feel about that? And private options? How much do they cost? What are their qualifications? Will they help with breastfeeding, or ‘snip and run’? What about follow up? Is it free or will you have to carry on paying?
6. Practitioners have different opinions on lots of things, from the best way to divide, what age of baby they will treat, whether they will do it at home or in a clinical setting, what tools to use, how much they charge (if in private practice), and what, if any, kind of aftercare and/or suck training the baby may need after division. The main thing to bear in mind is that there is very little research out there at all. We are living in a period of renaissance of knowledge so we’re feeling our way and working it out as we go along. Like any field, the large egos and loud voices are heard above the rest. It doesn’t necessarily make them right. One thing I have learned: every tongue tie story is unique and that pesky little frenulum may play a small or large part in a mother’s journey to successful breastfeeding.
7. Restriction equals tension. That tension may miraculously disappear with the tongue tie or it may not. Some tension may not even be caused by the tie but by birth trauma or position in utero. I, and many other breastfeeding supporters have seen cranial osteopaths work miracles. But it’s not particularly evidence based (if that’s important to the mother), expensive and doesn’t always work. Cranial osteopaths seem to come in all shapes and sizes, so listen to local recommendations from other mothers and breastfeeding supporters and go with your gut.
8. Parents going through breastfeeding problems need information and support; we all know that. Parents of tongue tied babies often have an additional layer of suffering: person after person telling them there is nothing wrong, or she’s doing it wrong, or her milk isn’t good enough, or her child needs drugs for reflux, or her child is lazy/stupid/doesn’t like her breasts, or her breasts are too big/small/nipple too big or small or fat or long (add your favourite fiction here). Conflicting explanations and the implied criticism that it is all the mother’s fault make tongue tie stories particularly heart-rending.
9. You may hear many opinions on why there seems to be a sudden epidemic of tongue tie. Maybe there are more of us spotting them. Maybe in days gone by, mothers would have struggled on, or given up or passed the baby around to give her nipples a rest – who knows. Maybe, eons ago, severely tied babies would not have survived infancy; thus not passing on their genetic predisposition. Perhaps there is some environmental cause for all these restrictive frenulums (research is underway so watch this space).
One thing is for sure: tongue tie is not the crazy-arsed invention
of loony middle-class breastfeeding supporters
giving their upper-class mothers
an acceptable excuse not to breastfeed
(yes, I really have heard that one)
So, maybe we ARE dividing too many. Maybe we’re letting thousands of mothers down who suffer but never find out a little snip might have helped them achieve their breastfeeding goals. There are a million and one questions to which we don’t have answers.
There are only two things I’m certain of:
1. I don’t believe anyone who says they know the answer and they can guarantee a positive outcome, if only you’ll do as you’re told. Beware towering egos!
2. Whatever strongly held opinions may be floating about, mothers deserve the best information we have (including what we don’t know and that division is not necessarily a magic bullet), have access to good quality, appropriate local treatment options and given space to make an informed decision.
Her body, her baby, her choice.

The tendency of the medical community to scoff at the notion that tongue tie can adversely affect feeding makes my blood boil! You are so right about the dyad needing to be seen, not just the baby (with a backhanded comment about the mother’s breasts thrown in). I have five children, and three of them have tongue tie, but only the youngest struggled to feed. In fact, I didn’t even know the older ones had ptt until we checked them after the baby’s diagnosis! She had her tongue tie divided at nearly 5 weeks but still needed topping up with ebm until she was 10 weeks old. Terribly stressful, and I only coped because I had fed my older ones and was confident enough to access as much support as possible. Most women in my position would not have soldiered on because it’s horrifically stressful to watch your baby’s weight go down and down every few days. I wouldn’t wish that experience on anyone, ever.